Tooth
Infection
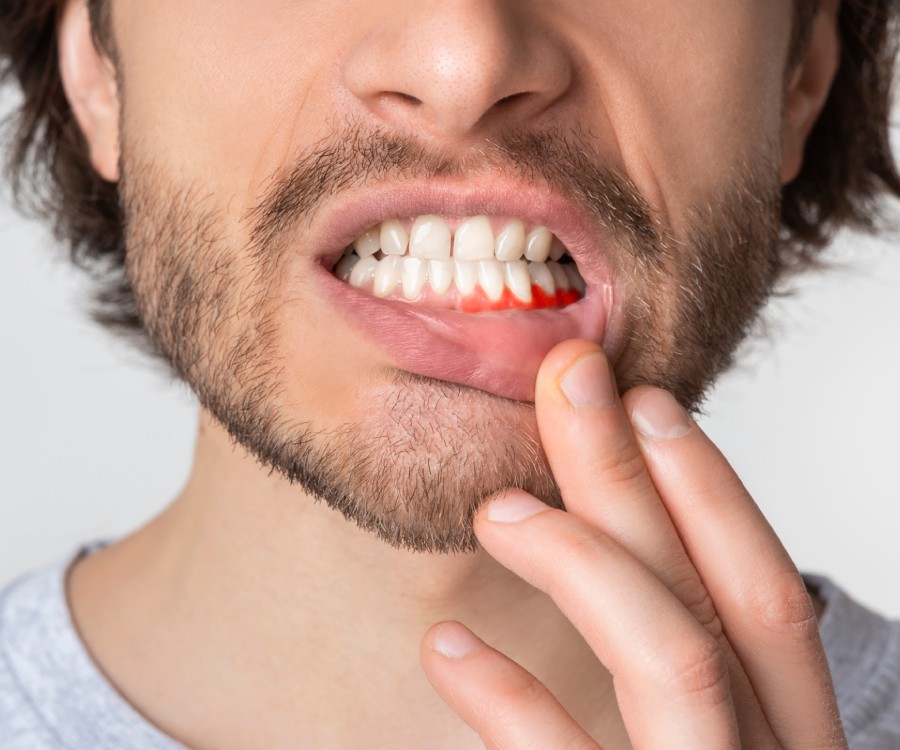
What is a tooth infection?
A tooth infection occurs when bacteria gets lodged inside a tooth. Once a tooth gets infected, it no longer has blood flow, which means that antibiotics can’t kill this bacteria. This is what makes a tooth infection different than any other infection in your body. A tooth acts like a petri dish and grows bacteria quickly. It can then pump this infection out into the surrounding tissues causing an abscess, swelling, pain and drainage. Let’s look at the various stages of a tooth infection.
Symptoms
Common symptoms of a tooth infection include swelling and pain in and around the tooth and gums. Symptoms can become severe and will typically get worse over time.
Other symptoms include:
- Sensitivity to hot and cold
- Pain that wakes you up at night
- Pain in your jaw, ear or neck
- Pain that gets worse when you lie down
- Pain when chewing or biting
- Redness
- Swelling
- Discolored or loose teeth
- Bad breath or taste
- Swollen lymph nodes in your neck or under your jaw
- Fever
In severe cases, swelling may affect your vision or breathing. These symptoms are extreme and severe. If you experience these, you should go to the emergency room right away.
Causes
Dental decay is the leading cause of tooth infection.
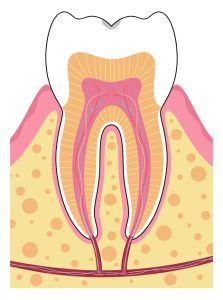
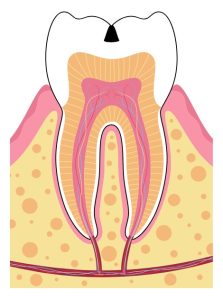
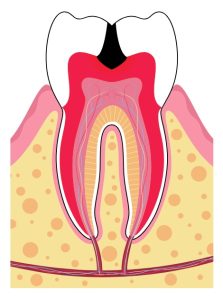
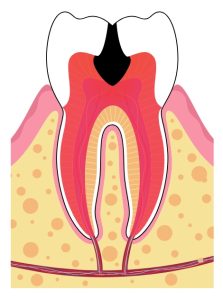
Millions of bacteria live in our mouth at any given time. Some bacteria is beneficial, while others can cause damage and destruction to teeth and surrounding bone. For this bacteria to get inside the tooth, it has to break through the enamel. The bacteria does this by consuming sugar (from your diet) and producing acid. Acid, over time, breaks down the tooth enamel and allows the bacteria to enter. Once the bacteria enters through the enamel, it reaches the soft inner dentin. This portion is much softer and breaks down eight times faster than the enamel. The innermost portion of the tooth is the nerve. As the bacteria starts to approach the nerve, it becomes inflamed in an attempt to fight off the bacteria.
Typically, when a tooth becomes inflamed, the vessels swell. Since the nerve is in a confined space, as it swells from inflammation, it can be extremely painful. Eventually, the nerve will die, and this extreme pain will subside. Even though the tooth might feel better, it is still filled with bacteria. The bacteria continues to multiply until it has nowhere else to go except for out the bottom of the tooth. As it pumps out the bottom, it creates an infection called a periapical abscess. The abscess can continue to grow around the teeth and into the adjacent spaces like inside the mouth, the sinuses and fascial spaces (the spaces between muscles, glands and organs). When the abscess grows in fascial spaces, it can cause dangerous infections that can spread through the body and even affect your breathing.
Other causes of periapical abscesses:
-
Trauma can cause a tooth to die. This is more common with front teeth. This process can be immediate, or it can take years to form an abscess. Typically, you can tell if it is abscessing if it hurts to tap or bite on the tooth.
-
A cracked tooth can also kill the nerve and start the process of abscess formation.
Other types of infections:
Bacteria can get stuck around the gums and form an abscess. Several types of abscesses can form around the teeth.
Periodontal abscesses occur due to advanced periodontal disease. Infections get stuck in pockets in and around the tooth.
A gingival abscess occurs when a foreign body gets stuck in the gum or between the teeth.
A pericoronal abscess typically occurs around a wisdom tooth when it doesn’t erupt correctly. If the tooth is impacted or partially erupted, an abscess is much more likely to occur.
When a tooth abscesses, it forms a pocket or bubble of infection (pus) due to bacterial infection. It can be extremely painful. Without treatment, the infection can grow and move into other parts of the body. In some cases, it can progress into a life-threatening issue.
Treatment
Treating an abscessed tooth depends upon the cause. This can be diagnosed with x-rays, CT Scans and by doing an intraoral exam. Once diagnosed, it can be properly treated. Typically, it is treated by removing the source of infection.
-
A periapical abscess caused by decay or trauma can be treated either by removing the inside of the tooth (root canal) or by extraction.
With root canal treatment, we remove the nerve and dead tissue from the inside of the tooth, thoroughly disinfect the inside, shape the canals and fill them with a rubber material to seal it off. This effectively saves the tooth allowing it to continue functioning normally.
With an extraction, we are removing the tooth that is infected. This will eliminate the cause as well; however, it is always better to save a tooth when possible. If there isn't sufficient tooth structure remaining to do a root canal, an extraction is necessary. However, going without a tooth long-term can cause other problems. An implant is recommended to restore form and function and prevent teeth from shifting.
-
A gingival abscess is caused by food stuck between the gums. Usually, the treatment consists of cleaning out the foreign body. We will disinfect the pockets with an antibiotic rinse as well. Sometimes a gingival abscess will need to be drained.
-
Typically, the only way to treat a periodontal abscess is to remove the tooth. We recommend a dental implant to replace a missing tooth so other teeth won't shift, and function is restored.
-
An impacted wisdom tooth causes pericoronitis. The treatment for this type of abscess consists of removing the wisdom tooth.

Complications
Even if an abscess has ruptured, it is still essential to have it treated. The source of the infection must be removed. If left untreated for a significant time, there is a risk that the infection can spread to other parts of your head, neck or brain. In rare cases, it can lead to life-threatening complications like sepsis. If you have a high fever, difficulty breathing or swelling near your eye, you should go to the emergency room before seeing us. These are signs of a severe, life-threatening infection.
Prevention
The best way to prevent infections is regular dental visits and good hygiene. Many times we can find these issues before they start.




